If you’ve already read our introduction to strokes, you now realize that there are different types of strokes, caused by different issues.
While ischemic strokes (the ones caused by a blood vessel blockage that impacts the brain) are the most common type of stroke, hemorrhagic strokes are typically more serious.
Hemorrhagic strokes not only have a lower survival rate than their counterparts, they tend to result in higher rates of lasting disability. And, the disabilities resulting from hemorrhagic strokes are usually more serious in their impact on functional abilities.
Here at WayWiser, we’re all about spreading awareness about issues that impact the lives of older adults, their families, and their loved ones.
Because the risk for stroke increases with age, it’s wise to enhance your knowledge about strokes, their symptoms, and risk factors.
Are you ready to become a stroke prevention warrior? Interested in enhancing your understanding of hemorrhagic strokes, ability to recognize their symptoms, and knowledge of what to do if you or someone you love ever experiences this type of stroke? If so, then this article’s for you.
Let’s explore everything you need to know about hemorrhagic strokes.
Here is what we’ll cover, in case you’d like to skip ahead:
- What is a Hemorrhagic Stroke?
- What are the Symptoms of a Hemorrhagic Stroke?
- What Are the Risk Factors for Hemorrhagic Stroke in Older Adults?
- How are Hemorrhagic Strokes Diagnosed and Treated?
What is a Hemorrhagic Stroke?
In general terms, a stroke involves interruption of blood flow to the brain. The brain requires a constant supply of blood to deliver the oxygen and nutrients it needs to function. A stroke impacts the flow of blood to the brain and its cells (neurons).
While the vast majority of strokes occur when a blood vessel that feeds the brain becomes blocked (known as an ischemic stroke), in around 13% of strokes, a blood vessel that provides fuel to the brain ruptures or develops a bleed. This is what happens in a hemorrhagic stroke.
This is also the key to why hemorrhagic strokes tend to be more serious and dire than their ischemic counterparts. Because, in addition to an interruption of cerebral blood flow, a hemorrhagic stroke also adds additional fluid into the mix, in the form of leaking blood.
There’s not much extra room in your head, so any extra fluid can quickly cause issues, as it doesn’t really have any place to go.
As a result, the buildup of blood can lead to pressure, irritation, and swelling of the brain and its surrounding tissues. And none of that is optimal when it comes to your brain’s health and wellbeing!
Reduced blood flow to your brain, blood where it shouldn’t be, and pressure build-up can wreak havoc on your brain’s cells.
These cells, known as neurons, are what your brain uses to send and receive information. They’re the building blocks behind every movement you make and thought you think.
When your neurons’ ability to function is impacted by a loss of blood flow, or a build-up of blood where it doesn’t belong—they begin to get sick and die off.
And that’s bad news, when you consider they’re the foundation of your brain’s abilities to do everything it does.
With any type of stroke, early identification and intervention are often key to both survival and optimal recovery.
That’s why it’s vital to ensure you know the common signs and symptoms of stroke, as well as the different types and why they occur.
Let’s explore the symptoms of hemorrhagic strokes.
What Are the Symptoms of a Hemorrhagic Stroke?

The outward symptoms of both ischemic and hemorrhagic strokes are often similar, but symptoms for hemorrhagic stroke can worsen drastically over time due to the ongoing and increasing pressure on the brain in this type of stroke.
Common signs and symptoms of hemorrhagic stroke include—
- Sudden onset of severe headache
- Nausea and vomiting
- Visual changes
- Light sensitivity
- Loss of consciousness (including fainting and coma)
- Dizziness and vertigo
- Stiff neck
- One-sided weakness or paralysis
- Speech and language changes (including aphasia and dysarthria)
- Seizure
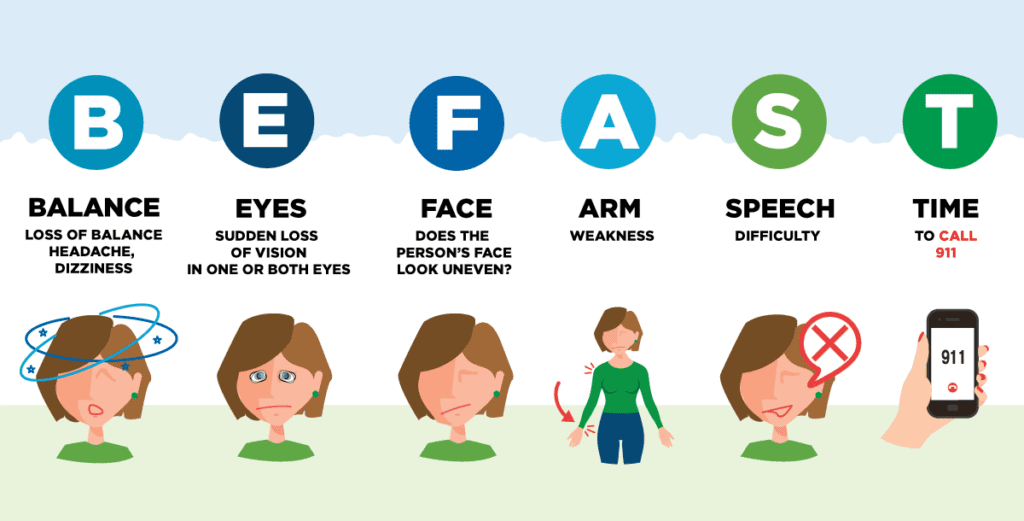
Using the stroke-identification acronym, BE FAST, is a helpful tool to recognize the signs of both ischemic and hemorrhagic strokes. But, it’s also important to be on the lookout for the additional indicators of hemorrhagic stroke that we’ve listed, above.
What Are the Risk Factors for Hemorrhagic Stroke in Older Adults?
There are two main types of blood vessel ruptures that lead to hemorrhagic strokes, each carrying its own set of risk factors. These types are—
- Intracerebral hemorrhage
- Subarachnoid hemorrhage
Let’s examine each subtype in greater detail.
What is an Intracerebral Hemorrhage?
Intracerebral hemorrhage, or ICH is the second most common subtype of stroke (behind ischemic strokes).
This type of stroke occurs when a blood vessel within the brain ruptures, impacting blood delivery to the brain and increasing pressure on the brain’s tissues.
The leaking blood, which is known as a hematoma, impacts the brain’s ability to send and receive information, by depriving its neurons of the oxygen and nutrients they require to function and survive, while also creating pressure and irritation within the brain’s sensitive tissues.
The longer the blood vessel bleeds, the larger the hematoma can grow, leading to increased symptom severity.
While you may expect ICH’s to occur more often during times of physical exertion or emotional stress, most occur during the course of normal, routine activities.
Though intracerebral hemorrhages account for less than 20% of all stroke occurrences, they have a higher case fatality rate than their ischemic counterparts.
Research shows that between 40% and 54% of ICHs prove fatal (between one month to one year post occurrence), and that between 12-39% of survivors achieve long-term independence, following an ICH.
While these statistics are sobering, it’s worth noting that many of the major risk factors for intracerebral hemorrhage are within your control to manage and minimize.
With awareness, support, and lifestyle changes, it’s likely you can make a positive impact on reducing your risks for intracranial hemorrhage.
Let’s look at risk factors and prevention strategies for intracerebral hemorrhage.
Reducing Your Risks for Intracerebral Hemorrhage

The most common cause of ICH is unmanaged high blood pressure (hypertension).
In developed countries, the statistics on ICH have improved with enhancements in blood pressure monitoring and control.
With diet and lifestyle modifications, medications, and expert support and guidance, many are able to get their blood pressure back to within normal limits, reducing their risks for ICH.
Other controllable risk factors for intracerebral hemorrhage include—
- Smoking
- Excessive alcohol consumption
- Illicit drug use
- Hypocholesterolemia
- Chronic kidney disease
Additional risk factors for ICH to be aware of include—
- Gender—ICH is more common in males than females
- Race—ICH is most prevalent amongst those of Asian ethnicity
- Age—your risks for ICH increase with age, with those aged 75 and older at highest risk
In addition, the presence of issues such as cerebral amyloid angiopathy (CAA), cerebral microbleeds (CMBs), and arteriovenous malformation (AVM) increase your risk for intracerebral hemorrhage. Unfortunately, these conditions don’t often present with overt outward symptoms, prior to causing an issue like an ICH. But they can usually be seen with brain imaging tests, and are relatively rare.
The biggest risk factors for ICH remain conditions that impact the circulatory system, with hypertension in the pole position.
What is a Subarachnoid Hemorrhage?
In contrast to a stroke caused by an intracerebral hemorrhage, a hemorrhagic stroke caused by a subarachnoid hemorrhage involves a blood vessel rupture in the cushioning that surrounds the brain and helps to keep it safe and secure.
Your subarachnoid space contains many major blood vessels that feed the brain.
Most subarachnoid hemorrhages are caused by a brain aneurysm that ruptures. The leaking blood can cause compression of the brain tissue, irritation, and neural death.
A ruptured brain aneurysm in the space between the brain and its cushioning layers is the cause of the majority of subarachnoid hemorrhages (also known as SAHs).
Another common cause of subarachnoid hemorrhage is traumatic brain injury. These injuries are most often sustained as the result of a car accident, fall, or blow to the head.
The most common symptom of a subarachnoid hemorrhage is a sudden and severe headache.
Known as a thunderclap headache, this type of headache strikes quickly and intensely. The other common outward signs of subarachnoid hemorrhage are aligned with those we’ve outlined, above.
Risk factors for developing a SAH include—
- Gender—females are at greater risk than males for developing this condition
- Genetics—those with a family history of ruptured aneurysm or SAH are at increased risk
- Lifestyle—as with ICH, those who smoke, consume excessive amounts of alcohol, or have unmanaged hypertension are at increased risk for SAH
- Medical Issues and Medications—those with estrogen deficiency, moyamoya disease, as well as those who take sympathomimetic drugs, or receive antithrombotic therapy are at increased risk for SAH
- Occupational or Recreational Hazards—those whose careers or hobbies involve an elevated risk for head injuries are at increased risk for SAH
Now that you’ve learned much about the causes, risks, and types of hemorrhagic strokes, let’s explore how they’re diagnosed and treated.
How are Hemorrhagic Strokes Diagnosed and Treated?

If you or someone you love experiences symptoms of a hemorrhagic stroke—prompt medical treatment and care are essential to improving the chances of survival and recovery.
If you recognize stroke symptoms in yourself or another, dial 911 and get to the nearest emergency department as soon as possible.
A rapid medical response is vital when it comes to hemorrhagic strokes, because symptoms tend to worsen over time as the pressure on the brain builds and the area of damage spreads.
The first goal of medical professionals when treating a hemorrhagic stroke is to save your life.
The next is to manage and minimize your symptoms and help your condition to stabilize.
Methods used in the initial response to a suspected hemorrhagic stroke may include—
- The use of life support equipment if necessary
- IV medications (which may be used to address issues such as blood pressure, anxiety, pain, swelling, and risks for complicating issues like seizures or artery spasms)
Once your condition has stabilized, medical professionals will assess the nature of the issue, to determine if a hemorrhagic stroke is the cause of your condition.
This typically involves assessment with brain imaging tools like—
If you’re conscious, your healthcare provider may ask you questions to assess your neurological status. If not, they’ll assess your reflexes and check your pupils and involuntary responses. Blood may be drawn for testing.
Because hemorrhagic strokes are difficult to treat directly, the primary goals of acute care for this condition are to lower and control blood pressure, and reduce further bleeding.
In some cases, brain surgery may be necessary to address the source of the stroke and improve chances for recovery.
The average hospital stay following a hemorrhagic stroke is anywhere from 10-20 days, depending on need.
Following the acute care phase of treatment for hemorrhagic stroke, most survivors will undergo a lengthy recovery journey, focused on regaining their prior level of independence and functioning.
Recovery from hemorrhagic stroke involves a team of rehabilitation professionals, working to improve mental and physical functioning.
- Speech and language pathologists (SLPs) work with people recovering from strokes on improving their speech, language, cognitive, memory, voice, and swallowing skills.
- Physical therapists (PTs/PTAs) assist with improving strength, range of motion, balance, endurance, safety, and coordination skills.
- Occupational therapists (OTs, OTRs, OTAs, COTAs) are focused on improving the safe and independent performance of activities of daily living, as well as hand and finger strength and range of motion. They’re also your go-to therapists for the development and training of any adaptive equipment needed.
Rehabilitation may also involve mental health professionals, to address any issues with depression, anxiety, and other behavioral changes.
Intensive therapy following a hemorrhagic stroke helps to improve safety, function, quality of life, and life expectancy.
In some cases, medications are used to support recovery and manage symptoms, but this depends on individual factors and will be determined by your medical team.
Because research shows the outcomes for those who experience hemorrhagic stroke are not optimal, it’s wise to work to prevent this issue through understanding personal risks and managing those within your control to address. It’s also important to be able to identify them if they occur, to get prompt medical care for yourself or a loved one.
As the saying goes—”An ounce of prevention is worth a pound of cure.”
When it comes to hemorrhagic strokes, this expression is your guiding light.
While research shows the fatality rate from hemorrhagic strokes may be decreasing, it’s proactive to manage any modifiable risk factors you or a loved one may have, to avoid this issue ever impacting your life or family.
WayWiser is passionate about supporting older adults and their loved ones to live happier, healthier lives. Our product offers exclusive benefits you won’t find anywhere else. Visit our Word to the Wise blog regularly for new content on topics that matter to you. Stay connected, protected, and wise.







