Did you know that stroke is the fifth leading cause of death in the United States? It’s also a major cause of long-term disability in Americans. Each year, nearly 800,000 Americans experience a stroke. And the most common type of stroke is the Ischemic Stroke.
While these statistics may seem ominous, they’re not presented to frighten. But it is important to be aware of just how many American lives are affected by stroke.
If you or someone you love experiences a stroke—you’re not alone. If this issue hasn’t impacted your life, there’s much you can do to minimize your risks for ever having one.
For a full introduction, check out our Ultimate Introduction to Strokes.
So, what is an ischemic stroke, anyway?
Why are they so common?
What can you do to prevent one, in yourself or someone you love?
This article will answer these and more questions about ischemic stroke.
Here is how it’s laid out:
- What is an Ischemic Stroke?
- What are the Different Types of iIchemic Strokes?
- What Are the Signs and Symptoms of Ischemic Stroke?
- What to do in the Event of an Ischemic Stroke
- What Are the Risk Factors for Ischemic Stroke in Older Adults?
- How Are Ischemic Strokes Treated and Prevented?
Let’s dive right in.
What is an Ischemic Stroke?



Ischemic strokes are the most common type of stroke. They account for more than 85% of all strokes that occur.
An ischemic stroke is the result of a blood vessel blockage.
Medically, a stroke is known as a cerebrovascular accident (often abbreviated as CVA). It’s what happens when a blood vessel that interfaces with your brain is stopped from fulfilling its duty of supplying blood to your brain.
Ischemic strokes occur most often when an artery that feeds the brain becomes blocked by a blood clot or piece of plaque debris.
When this happens, the brain is deprived of the steady flow of oxygen and nutrient-rich blood its cells need to function.
Your brain cells (known as neurons) require a constant supply of blood to do their very important work of sending and receiving information. Starved of their essential fuel, they begin to get sick and die off.
The longer the blood flow is interrupted, the more neurons are impacted—and the less likely they are to recover.
Research from UCLA discovered that two million brain cells are injured each minute during a stroke. The longer a stroke goes untreated, the greater the damage to your brain, as more and more neurons become impacted.
This is the crux of why time is of the essence when it comes to stroke treatment. The longer your brain goes without the blood supply it needs—the worse the potential outcomes get.
That’s why the phrase, ”Time lost is brain lost”, is a common pronouncement in the stroke awareness community.
Recognizing ischemic stroke symptoms and getting prompt medical treatment are key factors in stroke survival and recovery prospects.
But how do blood vessels in the brain become blocked and cause an ischemic stroke?
There are two primary ways this occurs. Let’s take a look at each, to enhance your awareness of how and why these types of strokes occur.
What Are the Different Types of Ischemic Strokes?



Ischemic strokes are divided into two main subtypes, depending upon where the offending blood vessel blockage originates.
Thrombotic ischemic strokes occur when a blood vessel in the brain becomes blocked. “A thrombosis thrives where it is” is a helpful way to remember the specifics for this type of ischemic stroke.
Embolic ischemic strokes occur when a piece of material (blood clot or plaque debris) that develops in an artery in the body breaks free and travels to the brain, where it causes a blockage. You can use “an embolism embarks on a journey” to remember the origins of this type of ischemic stroke.
Some researchers also further classify ischemic strokes based on their underlying causes.
These etiology-based categories for ischemic strokes include—
- Cardioembolic
- Atherosclerotic
- Lacunar
- Other known causes, including—
In some cases, the underlying cause of an ischemic stroke is unclear. Known as cryptogenic strokes, this is the classification for strokes with unknown causation. Here’s a helpful handout that explains more about cryptogenic strokes.
Even though there are many different ways ischemic strokes occur, the outward signs and symptoms are often similar. Let’s review the common signs and symptoms of ischemic stroke, so you can feel empowered to recognize one if it happens.
What Are the Signs and Symptoms of Ischemic Stroke?



While it’s true that no two strokes are exactly alike, ischemic strokes often present with common outward signs that can help you identify them if they occur.
The American Stroke Association coined the widely-used acronym, Act FAST, to assist in stroke symptom identification. The letters in this stroke recognition tool stand for—
F—Face. Is one side of the face drooping or numb? When the individual sticks out their tongue, does it noticeably deviate toward one side?
A—Arm. Is one arm numb, weak, or hanging down? When the person attempts to lift both arms down one drift downward?
S—Speech. Is the individual having difficulty speaking, finding the right words, or using speech patterns that are garbled, slurred, confused, or nonsensical?
T—Time to call 911! If you notice any of the above issues, get medical assistance as soon as possible. Remember—time lost is brain lost.
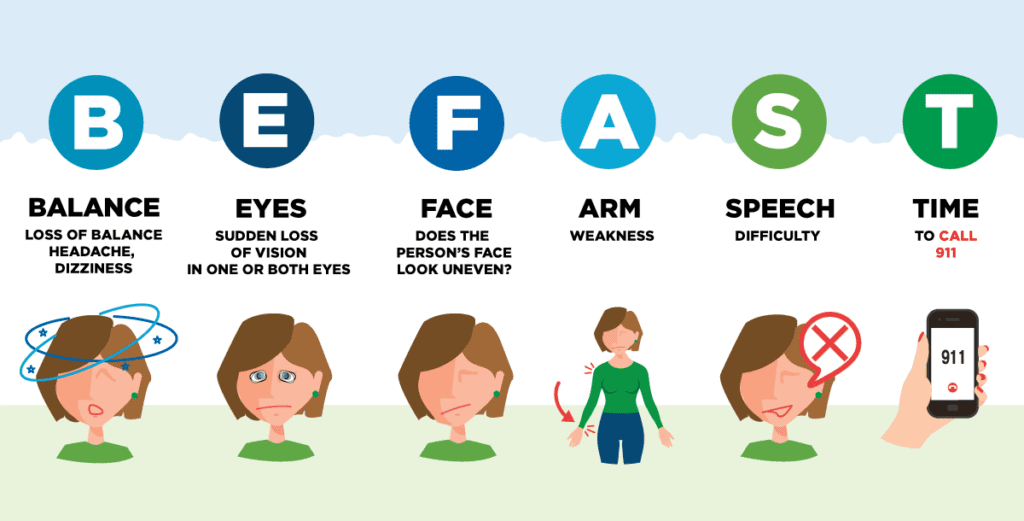


Additional signs of ischemic stroke include confusion, sudden headache, vision issues, balance and coordination difficulties, and one-sided numbness or weakness in the body.
What Are the Risk Factors for Ischemic Stroke in Older Adults?
Risk factors for ischemic stroke are usually broken down into a few categories, depending on whether they’re the result of medical conditions, lifestyle choices, or unmodifiable statistics that are known to contribute to increased risk for stroke, such as age.
Medication conditions that increase risks for ischemic stroke include—
- High blood pressure (hypertension)
- High cholesterol
- Atrial fibrillation (Afib)
- Diabetes
- Atherosclerosis
- Carotid artery disease
- Heart disease
- Peripheral artery disease
- Sickle Cell Disease
- History of stroke or transient ischemic attack (TIA)
Lifestyle factors that contribute to risks for ischemic stroke include—
- Smoking
- Excessive alcohol consumption
- Sedentary lifestyle
- Obesity
- An unhealthy diet
Other factors known to contribute to increased risk for stroke include race, gender, and a family and personal history of strokes. Even though these factors can’t be changed, it’s still important to be aware of their impact on your risks for stroke.
How Are Ischemic Strokes Treated and Prevented?



The best news about ischemic stroke prevention is there’s a lot you can do to reduce your risks for one.
Many of the major risk factors for this type of stroke are within your power to manage and minimize with lifestyle changes, medications, and healthcare support.
Lifestyle changes that support your heart and circulatory system health and wellbeing are a powerful way to reduce your risk for an ischemic stroke.
Working with a healthcare team to address, support, and manage any medical conditions associated with increased stroke risk is also an important part of stroke prevention.
This can include taking medication for blood pressure or high cholesterol, and could also involve daily monitoring of blood pressure, or performing blood glucose level checks.
Your doctor and healthcare team will be able to advise you on necessary stroke prevention steps you should be taking, and why they’re important to manage your personal risks for stroke.
What to do in the Event of an Ischemic Stroke



If you or someone you love are showing signs and symptoms of a stroke, it’s vital to know what steps to take to enhance chances for survival and recovery.
While it may seem appropriate to drive yourself or your loved one to the hospital, the wisest course of action (and the one encouraged by medical professionals) is to dial 911 and get to the nearest hospital via ambulance.
Why is this optimal?
- Because EMS can perform life-saving measures enroute to the emergency room
- Arrival to the ER in an ambulance may secure faster treatment
- Your EMS responders may divert you to a specialized stroke treatment center if available and appropriate
- Plus, your emergency medical response team will collect important information that will inform and streamline your treatment process once you arrive at the hospital.
Remember—every minute matters when it comes to a stroke. Dialing 911 in the event of a stroke can provide you with extra life-saving minutes that often make all the difference.
Here’s a helpful, print-friendly article from the Centers for Disease Control (CDC), explaining why EMS is your best first line of defense in stroke care and treatment.
The treatment protocol for ischemic stroke depends on the individual, and the location and severity of the stroke in question.
The first goal of treatment is to save a life, to achieve medical stability, and to reverse the effects of the stroke with medical interventions.
When it comes to stroke treatment, there’s a healthcare concept known as the three-hour window. During this timeframe, treatments are most effective and more options are available for treating a stroke.
If you make it to the hospital within this three hour timeframe, your medical team may be able to administer thrombolytic drugs. These clot-busting meds are used to break up and dissolve the blood clots that are causing the stroke.
The quicker your blood can start moving again, the quicker your brain will get the oxygen it needs. This helps to minimize and even reverse the damage caused by a stroke. But it all depends on timing.
In some cases, blood thinning medications and surgical interventions will be part of a hospital treatment course for ischemic strokes.
Once the acute care phase of ischemic stroke treatment is completed, recovery is often ongoing.
Many people receive continuing care at skilled rehabilitation centers and skilled nursing facilities, in order to maximize their functional recovery from a stroke.
Skilled therapists involved in stroke recovery and rehabilitation include physical therapists, occupational therapists, and speech-language pathologists.
These skilled professionals create individualized treatment plans to promote recovery of functional skills, with the goal of regaining independence to the fullest extent possible.
Stroke rehabilitation therapists focus on targeting the reacquisition of skills like—strength, coordination, speech, cognition, swallowing, language, fine motor skills, self-care, safety awareness, and mobility.
Here’s a link to a helpful list of stroke recovery resources, for patients and their families, from the American Stroke Association.
Other vital aspects that fuel the most successful stroke recoveries include family involvement, patient motivation, and the desire for education and advocacy.
Now that you know more about how ischemic strokes happen and how you can take steps to prevent one in yourself or a loved one, we hope this enhanced awareness will bolster your confidence in stroke prevention and recognition strategies.
After all, when research tells us that around 80% of strokes are preventable with lifestyle modifications and risk awareness strategies—you are the key to your health and wellbeing when it comes to stroke.
Use your power to reduce your risk for stroke, and your knowledge to educate and support those you love in minimizing theirs. Your brain will thank you.
If you’re curious, we also offer a similar guide to Hemorrhagic strokes and an Ultimate Introduction to Strokes in general.







